Pruritic skin disease is a common and frustrating problem encountered in primary care veterinary practice. One report by Hill (2006) indicated that pruritic skin disease accounted for 30–40% of dermatological problems in first opinion practice. Veterinary nurses play a dual role in the management of pruritic skin disease, to both help with the investigative process and also to advise owners on supplementary therapy that can help to make their pet more comfortable. While the presence of ectoparasites and infection are important causes of pruritus in the dog, once these and a food allergy (now more accurately referred to as cutaneous adverse food reactions, CAFR) have been ruled out, a diagnosis of atopic dermatitis can be made by exclusion. Canine atopic dermatitis (CAD) has been shown to affect the quality of life of both dog and owner (Linek and Favrot, 2010), not just because of the intense irritation that many dogs suffer with CAD, but because of the chronic nature of the disease and the tendency for dogs to have repeated relapses even though they may appear to be well controlled for long periods. The author is a strong advocate of veterinary nurse dermatology clinics to help support owners and manage their pet's skin disease.
Therapy for CAD can be divided into foundation and supplementary treatments. Foundation treatments are needed in most cases of CAD and will be not be discussed in any detail in this article. Foundation drugs are POM-Vs, offer good control of a high proportion of animals with CAD and have a strong evidence base to support their use. They include allergens specific immunotherapy, ciclosporine, glucocorticoids, lokivetmab and oclacitinib. Supplementary treatments, which includes antihistamines, essential fatty acids and topical therapy, rarely control anything but the mildest cases of CAD, but despite that, these drugs play an important role in the overall management of cases. They contribute to therapy by helping to improve skin and coat condition to reduce the levels of foundation drugs that are needed, and they help to reduce the incidence of atopic flares. This article will discuss some of the supplementary drugs that are readily available and do have some evidence to support their use and how their use may be advised by the veterinary dermatology nurse.
Antihistamines
A range of antihistamines have been described for use in CAD. Although there are anecdotal reports to suggest that antihistamines play an important role in the control of CAD there is only very limited evidence to support this recommendation (Scott and Miller, 1999; Zur et al, 2002). A critical review of the literature by the American College of Veterinary Dermatology (ACVD) task force on the use of antihistamines in the treatment of CAD confirmed this view (DeBoer and Griffin, 2001). This study revealed that the majority of published peer-reviewed trials were open, uncontrolled or partially controlled with efficacy rates ranging from 0–75%. Similar conclusions were reached by a later review by Olivry (2003). Antihistamines are divided into two classes (H1 and H2 antihistamines) based on the type of receptor they target. H1 antihistamines are used mostly to treat allergic disease and mast cell-mediated disease; H2 antihistamines are indicated primarily for gastric reflux disease due to their action on H2 receptors in the gastric mucosa. H1 antihistamines can be further divided into first and second generation drugs. First generation drugs have a central effect and therefore have a strong sedative action, they also produce anticholinergic side effects. Sedation can be a benefit in some dogs with atopic dermatitis especially if they have nocturnal pruritus. Second generation drugs tend to be less sedating and are used more commonly in humans for their anti-allergy effects. While owners should be discouraged from self-prescribing medication to their pets as not all human antihistamines have been shown to be safe in dogs, two antihistamines that are widely available in the UK for use by clients are chlorpheniramine and cetirizine. Both are available as over the counter purchases and exist as both branded and low cost generic drugs.
Chlorpheniramine maleate is a first generation alkylamine antihistamine. It is indicated as therapy in dogs with histamine-mediated pruritus and allergic skin disease. It can be heavily sedating in some animals. It is normally prescribed at doses of 4–8 mg per dog to a maximum of 0.5 mg/kg, orally two or three times daily, and is available in both tablet and liquid formulations. Although undoubtedly many owners claim that their pets do derive significant benefits from this drug there is little other than anecdotal evidence to recommend its use as a mono-therapy in allergic skin disease in dogs. Given within the recommended dose bands it is a relatively safe drug and providing there are no concurrent comorbidities or therapies to contradict its prescription, chlorpheniramine may be used for 7–10 days as a therapeutic trial to see if it can alleviate pruritus in allergic dogs.
Cetirizine hydrochloride is a second generation anti-histamine and tends to be less sedating than the first generation drugs such as chlorpheniramine. It is a piperazine derivative and a carboxylated metabolite of hydroxyzine with selective histamine H1 receptor antagonism. There are mixed reports of the benefits of cetirizine in the literature. One placebo controlled study showed oral dosing at 1 mg/kg controlled pruritus in 18% of dogs (Cook et al, 2004), however a second similar study using a higher dose of 3 mg/kg orally showed no significant difference between groups treated with placebo or cetirizine (Hsiao et al, 2016). The author's normal recommendation for the use of this drug would be as for chlorpheniramine. Providing there are no contraindications for it use a short 7–10 day trial is useful to assess any benefits.
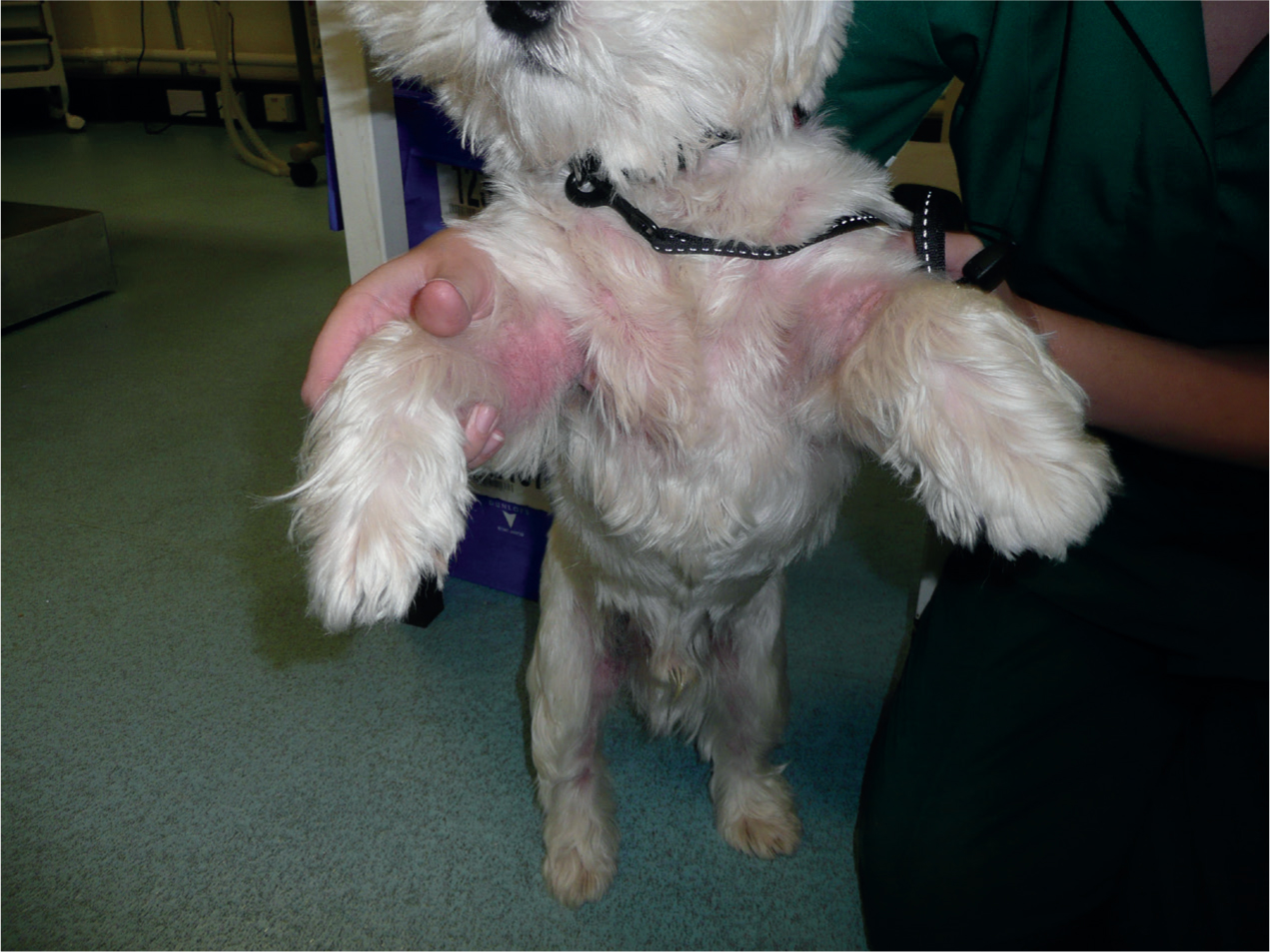
Both chlorpheniramine and cetirizine can help reduce pruritus in allergic dogs. Their use can be advised for a 7–10 day period to try and make animals comfortable either in the interim period while clients are waiting for a veterinary appointment or as a trial therapy before seeking more detailed investigation and veterinary advice (Figure 1). They must be withdrawn before in vivo allergy testing.

Essential fatty acids
Initial studies to investigate the benefits of essential fatty acids (EFAs) as therapy for CAD focused on their anti-inflammatory effects (Bond and Lloyd, 1992; Scarff and Lloyd, 1992; Scott et al, 1992; Bond and Lloyd, 1994; Paterson, 1995; Sture and Lloyd, 1995). EFAs are known to have the potential to affect allergic inflammation through the modulation of prostaglandin and leukotriene production (Olivry et al, 2001). Unfortunately many of the early trials reporting on the efficacy of oral EFA supplementation or EFA rich diets were poorly designed, exhibiting a range of deficiencies. These deficiencies included, but not exclusively, the lack of randomisation of trials; lack of blinding of investigators and/or owners; lack of placebo controls as well as the lack of standardisation of basal diets or supplements which could provide additional EFAs to the prescribed supplements. As such there is limited evidence from the numerous early studies to recommend the use of EFAs for their anti-inflammatory action. However interest has refocused on EFAs as human and then canine studies have established that barrier defects play an important role in the pathogenesis of atopic dermatitis (Marsella, 2013). Skin barrier dysfunction leads to increased water loss from the skin surface and potentially increased allergen penetration and sensitisation. Both lipid (e.g. ceramides) and protein (filaggrin) abnormalities have been described in CAD (Marsella et al, 2011; Marsella, 2013). More recent studies have assessed both topical (Blaskovic et al, 2014; Marsella et al, 2017) and oral administration of EFA. The latter as both supplements and in enriched EFA diets (Olivry et al, 2010; Popa et al, 2011). One study assessing benefits of a high EFA feed supplement showed that supplementation with omega-6 and omega-3 EFAs led to an overall increase in lipid content of the stratum corneum of atopic dogs and a significantly improved organisation of the lamella lipids in the lower stratum corneum comparable to healthy dogs (Popa et al, 2011). These recent finding suggest EFAs may play a role in improving barrier function in CAD, however further work is needed to demonstrate a definitive benefit. While the use of EFAs as sole therapy is questionable, they have been shown to have significant effects in reducing levels of foundation therapy when used in combination with both glucocorticoids or ciclosporine (Saevik et al, 2004; Muller et al, 2016). One study by Muller et al (2016) demonstrated that when EFAs were given in combination with ciclosporine the median daily ciclosporine dosage/kg bodyweight decreased significantly from 4.1 mg to 2.6 mg compared with 3.5 mg to 3.3 mg in the placebo group (Muller et al, 2016). The glucocorticoid sparing effect of EFAs was shown by Saevik et al (2004) who reported a significant reduction in pruritus scores in atopic dogs on combination therapy with both drugs compared with glucocorticoids alone. The improvement though did take 64 days to become apparent suggesting the benefits take time to become significant (Saevik et al, 2004).
EFAs do have the potential to reduce pruritus and improve skin and coat condition, however because of their very slow onset of action they are not suitable as initial therapeutic options in a pruritic dog. They can be useful as additional therapy in dogs on a treatment protocol, to help reduce the levels of concurrent drugs or improve the overall level of control.
Topical products
Topical products are important in all cases of CAD. While they are rarely able to be used as the sole form of long-term therapy, they do have the ability to contribute to the overall level of control of clinical signs and can help to reduce the levels of systemic drugs needed. Topical products can be used in the form of shampoo therapy or as leave on products such as creams, gels, lotions, spray and mousses/foams. Although shampoo therapy is time consuming it has the advantage of cleansing and hydrating the skin. The actives within shampoos can also be applied to large areas of the skin. Leave on preparations are quicker and easier to use than shampoos, but have the disadvantage that they can leave a residue on the skin which can make it feel slightly sticky. The author will commonly use a weekly regimen in allergic dogs that consists of twice weekly antipruritic shampoo therapy followed on each occasion by a moisturising mousse or spray with a leave on moisturising spray or mousse used between shampoo treatments to provide additional benefits.
Anti-pruritic topical therapy works in a range of different ways (Table 1). Drugs with specific anti-inflammatory activity include the glucocorticoids and calcineurin inhibitors, these POM-V drugs will not be discussed in this article.
Table 1. Mode of action of most common anti-pruritic topical drugs
| Type of anti-pruritic drug | Drug |
|---|---|
| Neuromodulators | Menthol — stimulates TRPM8 receptors to create a cold sensation |
| Moisturisers, emollients and barrier protection | Humectants (non lipid emollients) — attract and hold water glycerine, lactic acid, urea, propylene glycol and chitosanide |
| Occlusives — prevent evaporation petrolatum, mineral oil | |
| Emollients — oils or lipids that provide partial hydration and occlusion sterols, lanolin, glycerol, glyceryl stearates, ceramides, free fatty acids, cholesterol | |
| Natural anti-inflammatory agents | Oatmeal, aloe vera, calamine |
TRPM8 = transient receptor potential melastatin 8
Topical neuromodulators act to control pruritus by overriding the sensation of itch with another sensation. One of the best examples of this type of drug is menthol. Menthol stimulates specific receptors in the skin called transient receptor potential melastatin 8 (TRPM8) receptors to generate the perception of cold. This has very potent anti-pruritic effects. For this reason menthol is a common component of anti-pruritic canine veterinary products.
Numerous human studies have shown that moisturisers and emollients play an important role in restoring barrier function. Newer products have been shown to confer protective effects on skin barrier by delaying onset and decreasing the severity and numbers of flares of human atopic dermatitis cases (Danby and Cork, 2010). Moisturisers can be classified as occlusive, humectants (non-lipid emollient) or emollients (lipid) or combinations of the three. Many veterinary shampoos, mousses and sprays contain a mixture of humectants and emollients. While there is considerable anecdotal evidence to suggest these types of product have significant anti-pruritic effects there is little in the veterinary literature to substantiate this. A single study by Bensignor (2018) demonstrated the benefit of hydrating foams containing oatmeal and essential fatty acids as part of the treatment regimen in CAD. Within the lipid category, moisturisers contain a variable mix of ceramides, cholesterol and free fatty acids. The category of moisturisers that has shown most promise in human atopic patients are the ceramide-dominant topical emulsions. These types of products focus on physiologic lipid replacement therapy, particularly ceramides, to restore a normal epidermal balance rather than the occlusive moisturisers which merely form an occlusive barrier on the skin. Ceramide dominant moisturisers are thought to permeate the stratum corneum and are synthesised in the keratinocytes, processed in the lamella bodies and secreted back into the stratum corneum to help repair the epidermal defect (Anderson and Dinulos, 2009). Topical lipids have been shown to improve barrier function in atopic dogs (Piekutowska et al, 2008; Popa et al, 2012), however the results from several clinical trials have revealed very variable results from topical products that produce good control (Fujimura et al, 2011; Blaskovic et al, 2014; Marsella et al, 2017) to those that offer little or no improvement (Hobi et al, 2017).
Natural anti-inflammatory drugs have been used for many years to help control pruritus. Oatmeal, aloe vera and calamine are three of the most common of these types of products. Colloidal oatmeal is a centuries-old topical treatment which has been used for a variety of human skin conditions, including skin rashes, erythema, burns, itch, and eczema. It is known to have moisturising properties as well as anti-inflammatory effects (Reynertson et al, 2015). Aloe vera has also been shown to have anti-inflammatory effects and is a component of several veterinary moisturising, anti-allergy shampoos (Feily and Namazi, 2009). Calamine lotion is a combination of zinc oxide and ferric oxide and is produced by adding other ingredients like phenol and calcium hydroxide. The zinc within the calamine has both anti-inflammatory effects due to its ability to inhibit mast cell degranulation and also has soothing properties (Gupta et al, 2014).
Topical therapy can provide immediate relief to dogs with pruritus (Figure 2). Just the action of shampooing a dog with cool water helps to hydrate the skin and reduce irritation. Every clinic should stock topical oatmeal moisturising shampoos and mousses that can be prescribed over the counter to make dogs more comfortable. The only real contraindication with shampoo therapy is the need to check the compatibility with topical anti-parasitic products, other than this medication can be supplied to owners with a high degree of confidence it will help their pet.
The role of the veterinary nurse
Many clients will seek out help from the veterinary practice nurse before agreeing to commit to a veterinary consultation for their pruritic dog. Others are apprehensive about returning for a follow-up examination after they have seen the veterinary surgeon and a diagnosis has been made, but where therapy has been only partially successful. In these circumstances a consultation with the veterinary dermatology nurse can advise clients on a range of things. This may be appropriate ectoparasite control or the institution of a hypoallergenic diet. Veterinary nurses may also advise on the use of symptomatic therapy where clients either cannot come in to see the veterinary surgeon or will not come in to see the veterinary surgeon. Topical therapy is particularly useful in these circumstances as it rarely fails to make animals more comfortable, even if that improvement is only temporary. Alternatively it is sometimes time spent with a client by the veterinary nurse, to explain the nature of their pet's disease and the need for consistent reassessments, that convinces them to come back for a recheck with their veterinary surgeon.
Conclusion
While there is a paucity of high quality evidence in the veterinary literature to provide a strong evidence base for the use of treatment such as antihistamines, essential fatty acids, non-steroidal anti-inflammatory drugs and topical anti-pruritic therapy, there is no doubt such drugs do contribute to the treatment of CAD. Nurses have the opportunity to contribute to the management of dermatology cases within their practices by advising clients on supplementary drugs that can help make their patients more comfortable.
KEY POINTS
- Supplementary therapy can be advised by the veterinary nurse to help in the management of allergic skin disease.
- Drugs such as antihistamines and essential fatty acids can be used to reduce the level of foundation drugs that are needed to control cases of canine atopic dermatitis (CAD).
- Topical treatment with moisturising products such as shampoos, sprays and mousses can help make pruritic dogs more comfortable.


