Glaucoma is a group of eye conditions that damage the optic nerve. Glaucoma can be a difficult ophthalmic emergency to treat and can be classified as primary or secondary.
Primary glaucoma
Primary (hereditary) glaucoma is a congenital abnormality causing a malfunction and malformation of the eye/s, reducing the flow of aqueous humour and often slowly increasing intraocular pressure over time (Reinstein, 2018). Generally, primary glaucoma is a bilateral disease affecting one eye initially, then the second eye 6–18 months later. Primary glaucomas can be further subdivided into two types: primary closed angle glaucoma and primary open angle glaucoma.
Primary closed angle glaucoma
Primary closed angle glaucoma (due to goniodysgenesis) is the most common primary glaucoma seen in dogs. Goniodysgenesis, also known as pectinate ligament dysplasia, pectinate ligament abnormality, or iridocorneal angle abnormality, is a dysplastic development of the draining structure. On examination it is visible as pectinate ligament dysplasia, with dysplasia worsening over time, while causing a reduction in flow of aqueous humour (Large and Busse, 2018), which is an inherited risk factor for development of primary closed angle glaucoma in dogs. The condition is graded 0–3 based on its severity – the higher the grade, the higher the risk of glaucoma (Davies The Veterinary Specialists, 2021). This can occur in any breed of dog; however, it is recognised more frequently in the following breeds: American Cocker Spaniel, Basset Hound, Border Collie, Dandie Dinmont, English Cocker Spaniel, English/Welsh Springer Spaniel, Flatcoated retriever, Golden Retriever, Great Dane, Hungarian Vizsla, Japanese Shiba Inu, Leonberger, Siberian Husky, Spanish Water dog and Welsh Terrier. Development of symptoms comes later in life and the degree of pectinate ligament dysplasia can worsen over time, with severely affected patients having an increased likelihood of developing glaucoma (Large and Busse, 2018).
Primary open angle glaucoma
Primary open angle glaucoma is also an inherited condition in dogs, but the increase in intraocular pressure is much more gradual than in primary closed angle glaucoma. Affected dogs do not tend to show the classic sudden signs of blindness or pain, but instead lose their vision more slowly over time, sometimes taking months or even years to develop (Davies The Veterinary Specialists, 2021). Breeds known to be affected by primary open angle glaucoma are Basset hounds, Petit Basset Griffon Vendeens, Shar Pei (Davies The Veterinary Specialists, 2021), Norwegian Elkhounds and Beagles (Large and Busse, 2018). Patients that are genetically predisposed should have their intraocular pressure measured with tonometry routinely to allow for early interception of disease.
Secondary glaucoma
Secondary glaucoma is a non-inherited condition and is caused by a physical obstruction to the flow of the aqueous humour (Reinstein, 2018). Obstructions can arrive from proteinaceous debris, red/white blood cells, lens luxations, iris adhesions or tumours (Reinstein, 2018) and complications from cataracts or cataract surgery. Inability of the aqueous humour to flow from the posterior to the anterior chamber causes a condition known as iris bombe, where pressures increase within the posterior chamber, resulting in anterior bowing of the peripheral iris (Figure 1).
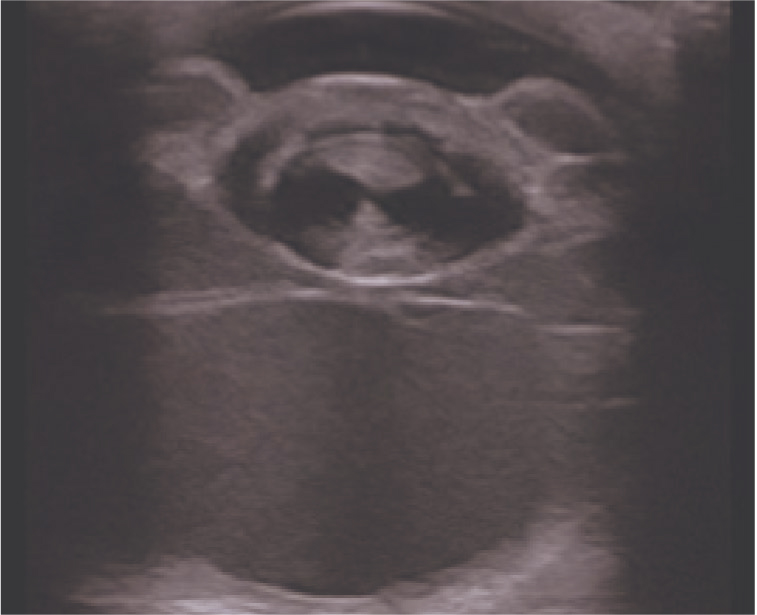
Clinical presentation of glaucoma
The onset of glaucoma can be acute or chronic, dependent on the speed of elevation of the intraocular pressure. Glaucoma can be asymmetric in both eyes of the same dog: one eye may be in a more advanced stage of disease, while the other shows no disease or early stages of disease. If acute case patients are treated medically within 12–24 hours of intraocular pressure increase, then vision is sometimes salvageable (Reinstein, 2018); however, glaucoma is a very difficult disease to treat and medical management is usually unsuccessful, with the outcome being that enucleation of one or both eyes is necessary. Emergency referral to a specialist ophthalmologist should be considered, to enable prompt diagnosis.
Acute clinical signs are usually more noticeable, and owners will report changes to the physical appearance of the eye as well as changes in generalised behaviour. Acute glaucoma can be extremely painful owing to the sudden dramatic increase in intraocular pressure (Gelatt, 2014). The patient may hold their eye shut or squint, and become head shy and protective of the face. Large and Busse (2018) mention that many dogs will suffer head or brow ache and develop changes in mentation, becoming dull, lethargic, depressed and inappetent.
Gelatt (2014) mentions that patients with chronic glaucoma are presented to practice later in the disease process, as the slower onset of clinical signs are less obvious to owners. These include sluggish or slightly dilated pupils, mild bulbar conjunctival venous congestion and early enlargement of the eye (buphthalmia or megaloglobus). The slower increase in intraocular pressure allows better tolerance of pain, with outward clinical signs of pain less noted by owners, meaning by the time these patients present to practice permanent vision damage is common. This is due to persistently high intraocular pressure causing damage and deterioration to the retina (Reinstein, 2018).
Clinical signs associated with the eye/s are a red, dilated, fixed or sluggish pupil; bulbar conjunctival venous congestion; corneal edema; a firm globe, negative menace response and reduction or absence of pupillary light reflex responses. With prolonged increases of intraocular pressure, secondary enlargement of the globe, lens displacement and breaks in the Descemet membrane can occur (Gelatt, 2014).
Diagnostic and monitoring tools
Tonometry Tonometry is an essential tool for clinical management of glaucoma (Large and Busse, 2018). There are three types of tonometry: indentation, applanation and rebound. All produce pressure onto the cornea: the more force that is needed to ‘flatten’ the cornea the higher the intraocular pressure. Normal IOP pressure in canines is considered to be between the range of 10–25 mmHg. In patients with glaucoma, the intraocular pressure will be outside of this range. Intraocular pressure of over 40 mmHg will be extremely painful, and persistently high intraocular pressure of above 40 mmHg can result in blindness within hours (Large and Busse, 2018).
Multiple intraocular pressure measurements (curve) are more informative than a single measurement, as intraocular pressure is a biologic variable. Large and Busse (2018) mention that studies show 40% of elevated intraocular pressure readings were missed when only a single intraocular pressure measurement was taken. Thirty-hour intraocular pressure curves with readings every 3 hours prevent these increases being missed. Patients with suspected glaucoma should be admitted to hospital. Veterinary nurses can measure intraocular pressures with tonometry every 3 hours for a minimum of 24 hours, recording readings on both the affected eye and the unaffected eye to monitor the effectiveness of treatments and to ensure intraocular pressure levels do not start to increase in the unaffected eye (Large and Busse, 2018).
Repeated intraocular pressure measurements can cause superficial damage to the cornea, so care should be taken to protect the corneas with the use of lubricants and, if available, contact lenses can be placed.
In the hospital, the patient should be handled carefully to reduce excessive stress and any neck leads/slip leads/collars or neck/head restraint/extension must be avoided. Alternatively harnesses should be used, as any tension to the neck could further increase the intraocular pressure (Busse, 2012).
Gonioscopy
Gonioscopy is a non-invasive procedure performed to examine the drainage angle, and identify inherited abnormalities, which is useful in breeds that are predisposed to primary closed angle glaucoma and to diagnose primary glaucoma, especially when tonometry may be inconclusive.
Generally performed without dilating the pupil, topical anaesthesia is applied to the eyes, a lens called a goniolens is placed onto the cornea surface, allowing a better view of the drainage angle, which is observed with a portable biomicroscope slit lamp. Patients with goniodysgenesis primary closed angle glaucoma, or who have the risk of developing primary closed angle glaucoma, will have defective/abnormal drainage angles. Since 2016 a grading system of 0–3 has been used to determine the level of disease, and breeds at risk are checked every 3 years (British Veterinary Association, 2019). Other grading schemes also exist.
Ultrasonography
Ultrasonography is a non-invasive tool used for the evaluation of intraocular disease. Topical analgesia can be placed into the eye and an ultrasound probe used to look for abnormal structures that could be the cause of secondary glaucoma, such as retinal detachment. Ultrasound biomicroscopy uses probe frequency ranges of 20–60 MHz to visualise microscopic areas of tissue; however, this is generally only available in larger referral hospitals.
Emergency treatment of glaucoma
Given the many causes of glaucoma there is no set management strategy, so treatment choices will depend on the individual case. However, in all cases immediate medical intervention is required to reduce the intraocular pressure to ideally less than 20 mmHg within a few hours (Large and Busse, 2018). The aim is to reduce the pain the patient is experiencing, and to prepare the eye for potential surgical intervention. Reduction in intraocular pressure is achieved with systemic drugs, usually in a combination and administered via topical and intravenous routes. Drugs include:
- Prostaglandin analogues increase drainage of aqueous humour, and also rapidly reduce intraocular pressure by increasing uveoscleral flow (Dickens, 2016). Prostaglandin analogues are used in the management of primary canine glaucoma including use in emergency management of acute cases (British Small Animal Veterinary Association, 2017). Prostaglandin analogues are contraindicated in glaucoma secondary to lens luxation due to the possibility of causing malignant glaucoma (Dickens, 2016) and should be used with caution in patients that have anterior uveitis due to the drug causing miosis and it is proinflammatory (Mandell, 2011)
- Hyperosmotic agents, such as mannitol, reduce the formation of aqueous humour by reducing plasma flow through the ciliary body and causing dehydration of the vitreous (Gelatt, 2014). Used in the management of acute glaucoma, it begins to reduce intraocular pressure within 15 minutes of administration and lasts 3–8 hours after the infusion stops, diuresis occurs after 1–3 hours (British Small Animal Veterinary Association, 2017). It should be used with caution in patients with cardiac or renal disease, and in dehydrated patients
- Aqueocentesis/paracentesis is a surgical procedure performed to reduce intraocular pressure in emergency situations or when medical management is ineffective (Large and Busse, 2018). It is a procedure used as a last resort, as complications can arise including trauma to the iris, corneal ulceration, bleeding and introduction of infection. Aqueous humour is removed from the eye by centesis (using a fine bore needle). The main aim is to reduce the pressure immediately, then to continue with medical management. Aqueocentesis is also used to retrieve samples of aqueous humour for cytology to check for underlying causes such as uveitis or lymphoma (Large and Busse, 2018).
Maintenance therapy to control intraocular pressure
- Beta-blockers reduce the formation of aqueous humour via their effects on beta receptors present in the ciliary body. They are used in the management of acute glaucoma, and can be used alone or in combination with other topicals (British Small Animal Veterinary Association, 2017). Beta-blockers cause bradycardia and bronchoconstriction, and should be avoided in patients with cardiovascular disease and asthma (Reinstein, 2018). Monitoring of the cardiovascular and respiratory state of the patient should be done while on these medications, especially in small dogs
- Carbonic anhydrase inhibitors decrease the volume of aqueous produced. They reduce the intraocular pressure significantly (Mandell, 2011) by inhibiting the formation of bicarbonate ions within the ciliary body epithelium. Carbonic anhydrase inhibitors are used for control in all types of glaucoma, alone or in combination with other topicals (British Small Animal Veterinary Association, 2017)
- Analgesics will provide systemic pain relief for patients experiencing a rapid spike in intraocular pressure. The use of opioid analgesics, such as methadone and buprenorphine, are advised to improve patient comfort and compliance for administering medications and tonometry readings (Large and Busse, 2018).
Surgical intervention
Anterior chamber shunts (gonioimplants)
Anterior chamber shunts are the most common and effective surgical procedure for glaucoma patients (Bras and Maggio, 2015).
A surgical procedure, called a cyclophotocoagulation, is firstly performed, which aims to reduce aqueous humour formation by the destruction of the ciliary body. This can be achieved via a multitude of techniques, then a gonioimplant (shunt) is placed in the anterior chamber of the eye, which enables aqueous humour fluid to drain from the eye into the frontal sinus; a valve attached to the gonioimplant allows adjustment of the aqueous humour flow (Figure 2).
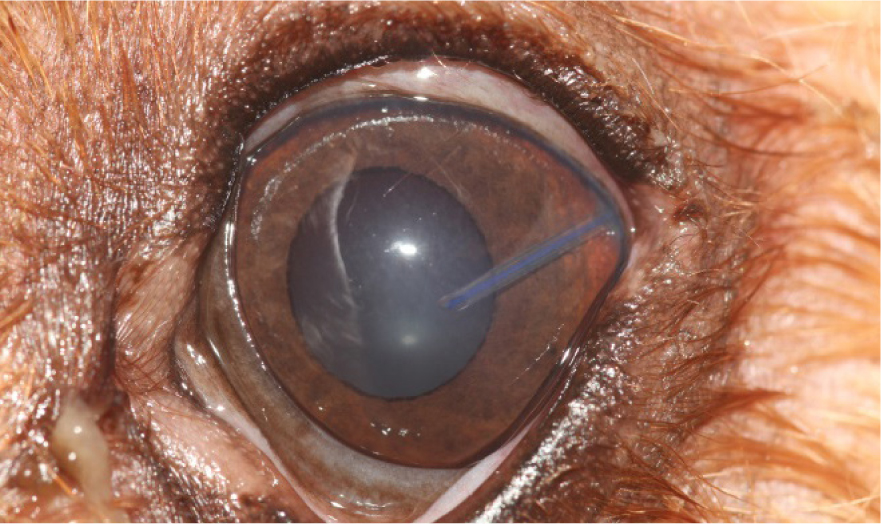
Candidates can be visual or blind and require general anaesthetic to perform this surgery. The aim is to remove the need for topical or systemic medications and to reduce pain.
Enucleation
In many cases where the intraocular pressure and pain cannot be controlled, or the vision is too damaged to correct with other techniques, surgical removal of the whole eye and eyelids is necessary for welfare reasons (Figure 3).

Once the eye is removed, the pain associated with glaucoma is removed. However, glaucoma can affect bilaterally, and removal of both eyes in this instance could affect patient welfare, so careful consideration should be made. Owners must be made aware of the likelihood of glaucoma development in the non-affected eye. The patient must have routine consultations to assess the health of the remaining eye.
Nursing care and monitoring of hospitalised patients
The process of nursing involves assessing a patient's needs, planning how they will be cared for, providing or implementing that care, assessing the response to that care and planning future care and reassessment (Main, 2011).
Patients with glaucoma tend to experience a degree of discomfort and pain as a result of the sudden onset of increased intraocular pressure (Large and Busse, 2018) or post-surgery. Assessment of pain is considered the fourth vital sign when examining a patient, alongside temperature, pulse and respiratory rate (WSAVA, 2014). The use of pain scoring tools can decrease subjectivity and bias, resulting in increased effectiveness of pain management, leading to better patient care (Epstein et al, 2015). Multiple types of pain scoring tools are available; however, it is useful to use the same pain scoring tool throughout the patient's treatment.
Opiates such as methadone or buprenorphine are analgesics of choice for management of acute pain (Large and Busse, 2018) and administration of analgesia every 4–8 hours (dependent on drugs used) depending on level of pain is vital to provide patient comfort. Under instruction from the veterinary surgeon, veterinary nurses can administer analgesia.
The most effective way to reduce pain in glaucoma patients is to reduce the intraocular pressure. This is generally achieved through management with topical medicines. Veterinary nurses should follow the medical plan carefully and ensure that all drugs are administered correctly and on time.
Routine intraocular pressure measurements are vital to tailoring treatment options for these patients.
Patients should be fitted with an Elizabethan collar to minimise self mutilation to the eyes, fresh water should be offered every 1–3 hours, and patients should be monitored when the collar is removed to eat and toilet. When using osmotic diuretics, such as mannitol, water should be withheld for 3–5 hours after initial treatment and the patient should be given regular opportunities to urinate (Whelan, 2014).
Prophylactic therapy
Prophylactic therapy of the fellow eye should be recommended. Betaxolol 0.5% (beta-blocker) every 24 hours delays the onset of glaucoma from an average of 8 months to 31 months in dogs (Reinstein, 2018). Combination therapy, regular monitoring and increases in frequency of topical treatments are commonplace, and owners need to be prepared and educated on the clinical signs of progressive disease and made aware that in nearly all cases, medical treatments will become less effective and potentially will fail over time, meaning and that their dog will likely lose one or both eyes (Reinstein, 2018). At-home tonometry is available for owners if they are confident in performing and recording the intraocular pressures. Owners need to be made aware of the risks of repeated tonometry on the cornea, with information given on corneal ulceration and the signs to look for. Regular examinations should be undertaken by the veterinary surgeon during this time.
Conclusions
Glaucoma can be a difficult ophthalmic emergency to treat. Even with prompt diagnosis and treatment, the outcome for the affected eye/eyes is poor, and many patients go on to lose one or both eyes. Accurate intraocular pressure reading and recording by veterinary nurses allows monitoring of clinical signs and allows treatments to be adjusted to individual patient needs. Pain recognition and prompt treatment improves patient wellbeing, and veterinary nurses play a crucial role in communicating the care required of these patients to their owners, post surgery and long term.
KEY POINTS
- Glaucoma is an ophthalmological emergency.
- Glaucoma is a very difficult disease to treat, and many dogs will require enucleation of the affected eye/s.
- Tonometry is an essential tool for the management of glaucoma.
- The most effective way to control pain in glaucoma patients is to reduce the intraocular pressure.


